The Value of Spreader Graft and Spreader Flap in Dorsal Reconstruction Following Hump Reduction in Primary Open Rhinoplasty in Tertiary Care Center
Abstract
Introduction: Resection of dorsal hump often leaves a widened, flat and open roof deformity, causing weakness at keystone area and diminishing the nasal valve angle. Incorporating spreader grafts or spreader flaps along the dorsum helps prevent these issues, providing both structural reinforcement and a restoration of dorsal aesthetic lines. The objective of this study was to identify the value of spreader graft and spreader flap in dorsal reconstruction following hump reduction in primary open rhinoplasty.
Methods: Prospective cross-sectional study conducted in the department of ENT-HNS of Kathmandu Medical College from April 2023 to March 2025. ROE questionnaire was used for aesthetic evaluation while NOSE scale was used for evaluation of functional outcomes. Descriptive statistics was used for comparative analysis of preoperative and postoperative ROE and NOSE scores.
Results: Preoperative ROE scores averaged (6.85 ± 0.69), rising markedly to (17.01 ± 1.14) at 3 months and (18.92 ± 2.08) at 6 months, demonstrating a statistically significant improvement (P < 0.001). In both the groups preoperative NOSE scale value was (42.29 ± 17.20), which showed marked improvement when re-evaluated at 3 months (29.55 ± 2.84), and 6 months (26.31 ± 2.19) postoperatively.
Conclusion:
In rhinoplasty, effective management to restore the nasal valve angle after dorsal hump reduction includes the use of spreader grafts or auto-spreader flaps. These techniques help to preserve or reconstruct the dorsal aesthetic lines while simultaneously supporting improved nasal patency and airflow for optimal functional results.
Keywords: Fiberoptic Laryngoscope (FOL), NOSE Questionnaire, ROE Questionnaire
Introduction
Rhinoplasty is a versatile surgical procedure performed to enhance nasal aesthetics along with improving airflow in patients affected by structural abnormalities such as septal deviation, nasal valve collapse, or turbinate hypertrophy.1 The internal nasal valve (INV) is the narrowest segment that contributes up to 50% of total airway resistance influencing nasal airflow.2 Dysfunction of the INV whether congenital, traumatic, or iatrogenic can significantly impair breathing and compromise surgical outcomes.
Preserving nasal function is a paramount in rhinoplasty. It is known that various rhinoplasty techniques, mainly osteotomies of the nasal bones, have the potential for altering the nasal airway. The Spreader grafts for reconstruction of internal nasal valve and to maintain dorsal aesthetic lines by placing grafts between the upper lateral cartilages and septum was pioneered by Sheen in 1980s.3 Sheen has used spreader grafts after hump resection to prevent the upper lateral cartilages from collapsing against the septum, thereby reducing the nasal valve angle collapse.
Auto-spreader flap is a new technique that gained more popularity recently and can be used as an alternative to spreader graft. The auto-spreader flap was described by Baker as a modification of Sheen’s spreader graft technique, whereby the dorsal aspects of the upper lateral cartilages are infolded and sutured to the nasal septum as a component of reduction rhinoplasty. This maneuver provides a cantilever-like effect on the internal nasal valve, while simultaneously achieving a smooth, even contour over the nasal dorsum.4-6 This technique avoids harvesting and carving cartilage for grafting from other locations. The objective of our study is to identify the value of spreader graft and spreader flap in dorsal reconstruction following hump reduction in primary open rhinoplasty.
Methods:
This is a prospective cross-sectional study among patients who visited the outpatient department of Otolaryngology-Head and Neck Surgery of Kathmandu Medical College from April 2023 to March 2025. Ethical clearance was taken from the ethical clearance committee of KMCTH. Patients undergoing primary rhinoplasty with dorsal hump and crooked nose were included in the study. Patients undergoing secondary rhinoplasty and with nasal polyposis and granulomatous diseases were excluded from the study.
All the patients enrolled in the study group were examined by consultant ENT surgeon. History regarding the cause of nasal deformity either congenital or traumatic nasal deformity was taken. Diagnostic Nasal Endoscopy using Fiberoptic Laryngoscope (FOL) was done to find out the type and grade of deviated nasal septum (DNS) and to rule out any associated nasal pathology. Rhinoplasty Outcome Evaluation (ROE) and Nasal Obstruction Symptom Evaluation (NOSE) questionnaire was used as an interview pre-surgery and post-surgery (3& 6 months) to find out the level of satisfaction and functional improvement respectively. The ROE questionnaire is composed of 6 questions and each question has five options between 0 and 4. For all six questions, the total score was calculated and the result was divided by 24 and multiplied by 100 (Zero represents minimum satisfaction and 100 the maximum one). A higher score indicates greater satisfaction. The mean ROE score < 50 are considered failures (unsatisfied), 50 to < 75 is considered good (partially satisfied), and ≥ 75 is considered excellent (highly satisfied).7 The NOSE (Nasal Obstruction & Symptom Evaluation) scale was introduced by Stewart et al.8 This is a disease specific quality of life instrument for subjective assessment of nasal obstruction. The NOSE score is calculated by summing the scores of the five questions and multiplying the total by 5, resulting in a score between 0 and 100. Higher scores indicate greater severity of obstruction. Scores are categorized into four levels: Mild (0–25), Moderate (30–50), Severe (55–75), and Extreme (80–100). A score of 30 or above is typically considered indicative of clinically significant nasal obstruction.
Data were entered in Microsoft Excel and analyzed using SPSS vs 20. Descriptive statistics were described by mean, median, standard deviation (SD) and interquartile range (IQR). Categorical variables were summarized using frequencies and percentages. Inferential statistics were performed using paired t-tests. A significance level of α < 0.05 was considered for all statistical analyses.
Surgical technique
Surgeries were performed under general anesthesia using an open rhinoplasty approach. Based on the specific patient’s nasal anatomy, non-randomized allocation method was used to subgroup the study group. An inverted V trans-columellar incision was made in the narrowest part of the columella and connected with a bilateral marginal incision at the caudal margin of the lower lateral cartilage. The flap dissection was performed in the supraperichondrial and subperiosteal planes until the nasal bones were reached. At the site of the anterior septal angle, septoplasty was done with the separation of connective tissue between the medial crura and the exposure of the caudal end of the septum. Before harvesting septal cartilage, the hump was addressed. Bony hump was removed by using rasps, drill, and 12 mm guarded osteotome, while cartilaginous hump reduction was done in component manner.
The spreader grafts
The spreader grafts were shaped in rectangular bars from harvested septal cartilage, approximately 2–3 cm long, 3–5 mm wide, and 1.5 mm thick. The next step of the nasal dorsum reconstruction was positioning of the harvested cartilages between the upper lateral cartilages (ULC) and the dorsal aspect of septal cartilage on both sides and in some cases of crooked nose, it was placed on one side only. The grafts were fixed to the septal edge at least twice; adjacent to the keystone area cranially and at the anterior septal angle caudally using 5-0 polydioxanone (PDS) sutures (Figure 1).
Auto-spreader flaps
Our modification of the spreader flap was in this step of surgery, where the bony hump was rasped, and the cartilaginous hump was preserved. Upper Lateral Cartilages were separated from dorsal septal cartilage. The cartilaginous hump was assessed and then transected in components. The mucosa was dissected from the medial side of the ULC and from the corresponding septal cartilage. ULC was folded inwards towards the septum and fixation of the ULC on to the side of dorsal septum by mattress PDS 5-0 sutures (Figure 2).

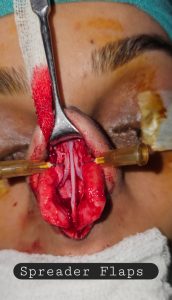
Figure 1 & 2: Showing use of Spreader graft and Spreader flaps respectively.
Results:
Sixty-two patients, 37 males (59.7%) and 23 females (40.3%), with mean age of 31 years, having persistent nasal obstruction and unhappy with the shape of their nose were included in our study. In 35 (56.45%) patients, spreader graft was used, while in 27 (43.54%) patients auto-spreader flap was used. Regarding the operative time for fixation of graft only, the auto-spreader flap was shorter in operative time (15.8 ± 3.4) minutes in comparison to the spreader graft (20.2 ± 3.2) minutes.
The overall aesthetic satisfaction was 74.2% (46 of 62) irrespective of the surgery done, but according to the surgical procedure, it was found that 25 (71.42%) of 35 patients treated by spreader graft were highly satisfied (ROE score >75), 8 (22.85%) patients reported partial satisfaction (ROE score >50<75) and 2 (5.71%) patients reported with unsatisfactory (ROE score <50) aesthetic outcomes. In patients treated by auto-spreader flap, 21(77.77%) of 27 patients were highly satisfied, 5(18.51%) of patients reported partial satisfaction, and 1(3.70%) patient reported unsatisfactory results (Table 1). The difference between two groups was not statistically significant (P >0.05).
The preoperative ROE score was (6.85±0.69) and postoperative ROE scores in 3 and 6 months were (17.01±1.14 &18.92±2.08), respectively, which were statistically significant (P<0.001). Functional assessment of nasal obstruction was done in all the patients using NOSE questionnaire. The preoperative NOSE score was (42.29 ± 17.20), which showed marked improvement when re-evaluated at 3 months (29.55 ± 2.84), and 6 months (26.31 ± 2.19) postoperatively. There was significant improvement in the patients’ symptom of nasal obstruction according to NOSE scale either treated by spreader graft or auto-spreader flap (Table 2).
Table 1: Showing number of patients with aesthetic satisfaction using spreader graft and auto-spreader flaps:
| Aesthetic Satisfaction (Number of Patients) | |||
| Surgical Technique | Highly Satisfied (ROE Score: >75) | Partially Satisfied (ROE score: >50-<75) | Unsatisfied (ROE score: <50) |
| Spreader Graft
35 (56.45%) |
25 (71.42%) | 8 (22.85%) | 2(5.71%) |
| Auto-spreader Flap
27 (43.54%) |
21 (77.77%) | 5(18.51%) | 1(3.70%) |
Table 2: Showing ROE and NOSE score before and after surgery.
|
|
Timepoint | ROE Score (Mean±SD) | Improvement (Δ) | p-value
(p<0.005) |
| Pair 1 | ROE score before Surgery
ROE score 3 months after surgery |
6.85±0.69
17.01±1.14 |
+10.16 | <0.001 |
| Pair 2 | ROE score before Surgery
ROE score 6 months after Surgery |
6.85±0.69
18.92±2.08 |
+12.07 | <0.001 |
| Pair 3 | NOSE score before Surgery
NOSE score 3 months after surgery |
42.29 ± 17.20
29.55 ± 2.84 |
-12.74 | <0.001 |
| Pair 4 | NOSE score before Surgery
NOSE score 6 months after Surgery |
42.29 ± 17.20
26.31 ± 2.19 |
-15.98 | <0.001 |
Discussion:
The removal of a dorsal hump is commonly done during a rhinoplasty.9 Complications noted in long-term follow-up include saddle nose, inverted V dorsal contour deformity and internal or external nasal valve collapse.10,11 The nasal valve insufficiency is frequently under-diagnosed and sub-optimally managed, despite its reported prevalence of 13% in cases with chronic nasal obstruction.12 Before proceeding with surgical correction, surgeon should emphasize the necessity of evaluating structural deformities and physiological contributors, including mucosal inflammation, if there is persistent nasal symptom even after septorhinoplasty.13 Due to aggressive hump reduction, insufficient upper lateral cartilage support, or postoperative scarring can reduce the INV to less than 10–15°, this complication can be effectively corrected with spreader grafts that widen the valve angle and stabilize the middle vault, enhancing both function and aesthetics.14
The role of spreader grafts in improving nasal airway patency and dorsal contour has been supported by clinical evidence, while Yoo and Most demonstrated that auto-spreader flaps maintain functional integrity along with aesthetic outcomes.15 We found no significant difference in early functional outcomes between spreader grafts and auto-spreader flaps, which is similar to the study done by Saedi et al.16 Unlike our study, Hassanpour et al.17 reported comparable aesthetic and functional results in-between spreader grafts and auto-spreader flaps. We found limitations in flap extension and inability to address the anterior septal angle for the auto-spreader flaps, which is similar to the study reported by Manavbasi et al.18
The analysis of spreader graft and auto-spreader flaps outcome using NOSE and ROE scores further supports their effectiveness. Statistically significant improvements were observed in both functional and aesthetic domains in our study. Comparative studies support these findings. A systematic review done by Keyhan et al. showed that both spreader grafts and auto-spreader flaps effectively restore dorsal aesthetic lines and improve nasal valve function, though spreader grafts demonstrated higher aesthetic satisfaction, which is consistent with our findings.19
A randomized controlled trial done by Naguib et al.20 found that spreader grafts provided better aesthetic outcomes, although auto-spreader flaps had shorter operative times which is similar to our study. Meta-analyses also show that in both techniques NOSE score improved significantly, but no statistically significant difference was found between them in terms of functional outcomes, which is in accordance to our study.19 This indicates that auto-spreader flaps is more preferable in cases requiring less invasiveness or shorter operative time, while for achieving optimal aesthetic refinement spreader grafts remain the gold standard. Moreover, auto-spreader flaps have gained popularity as a preservation technique, especially in primary rhinoplasty. A systematic review done by Garefis et al.21 concluded that auto-spreader flaps offer comparable functional and aesthetic outcomes to spreader grafts, particularly in well-selected cases.
We found visible irregularities on the nasal dorsum in some patients treated either with autospreader flaps and spreader grafts. Accurate placement and fixation of spreader graft was challenging task. Spreader grafts can become displaced if not properly sutured, leading to inverted “v” deformity or “saddle nose” deformity, or result in a wider bridge than desired. Sometimes, autospreader flaps were unable to provide sufficient dorsal width, especially compared to traditional spreader grafts. Precise scoring of autospreader flaps should be done, if scored too deeply can lead to collapse of the infolded cartilage, requiring actual spreader grafts. These were the limitations of our study.
Conclusion:
Dorsal hump removal in rhinoplasty may cause functional and aesthetic compromises because of excessive removal of cartilage and bone or disruption of keystone area. Long term complications such as INV dysfunction, saddle nose and inverted V deformity may be seen after hump reduction rhinoplasty. Both of these spreader grafts and auto-spreader flaps are effective in managing INV dysfunction as well as maintaining dorsal aesthetic lines. The choice of technique should be tailored to the patient’s anatomical needs, surgical goals, and the surgeon’s expertise. Our data aligns with broader literature, confirming that spreader grafts offer robust improvements in both nasal function and appearance, especially in cases requiring structural reinforcement and precise dorsal contouring.
References:
- Altidor A, Ferri FA, Bakhos F, Mascaro-Pankova A. Functional Rhinoplasty. Cureus. 2023 Sep 26; 15 (9):e45993. doi: 10.7759/cureus.45993. PMID: 37900451; PMCID: PMC10601979.
- Murthy VA, Reddy RR, Pragadeeswaran K. Internal nasal valve and its significance. Indian J Otolaryngol Head Neck Surg. 2013 Aug; 65(Suppl 2):400-1. doi: 10.1007/s12070-013-0618-x. Epub 2013 Jan 23. PMID: 24427685; PMCID: PMC3738809.
- Sheen JH. Spreader graft: a method of reconstructing the roof of the middle nasal vault following rhinoplasty. Plast Reconstr Surg. 1984; 73:230–239. doi: 10.1097/00006534-198402000-00013.
- Pepper JP, Baker SR. The autospreader flap in reduction rhinoplasty. Arch Facial Plast Surg. 2011 May-Jun;13 (3):172. doi: 10.1001/archfacial.2011.34. PMID: 21576664.
- Fomon SGJ and Caron AL (1950) Collapsed Ala. Acta Otolaryngologica, 51, 465-484. http://dx.doi.org/10.1001/archotol.1950.00700020488001
- Gruber RP, Park E, Newan J, Berkowitz L and Oneal R. (2007) The Spreader Flap in Primary Rhinoplasty. Plastic and Reconstructive Surgery, 119, 1903-1910.
http://dx.doi.org/10.1097/01.prs.0000259198.42852.d4 - Arima LM, Velasco LC, Tiago RSL. Crooked nose: outcome evaluations in rhinoplasty. Braz J Otorhinolaryngol 2011;77:510–5. https://doi.org/10.1590/S1808-86942011000400016.
- Stewart MG, Smith TL, Witsell DL, Weaver EM, Yueh B, Hannley MT. Development and validation of the Nasal Obstruction Symptom Evaluation scale. Otolaryngol Head Neck Surg. 2004; 130:157-63. doi: 10.1016/j.otohns.2003.09.016.
- Jang YJ, Kim JH. Classification of convex nasal dorsum deformities in Asian patients and treatment outcomes. J Plast Reconstr Aesthet Surg. 2011 Mar; 64(3):301-6. doi: 10.1016/j.bjps.2010.05.032. Epub 2010 Jun 29. PMID: 20591758.
- Karaaltin MV, Orhan KS, Demirel T. Fascia lata graft for nasal dorsal contouring in rhinoplasty. J Plast Reconstr Aesthet Surg. 2009 Oct; 62(10):1255-60. doi: 10.1016/j.bjps.2008.03.053. Epub 2008 Aug 21. PMID: 18722170.
- Burm JS. Correction of the Asian deviated nose with no hump using unilateral bony mobilisation and dorsal septal suture fixation. J Plast Reconstr Aesthet Surg. 2007;60 (2):180-7. doi: 10.1016/j.bjps.2006.03.038. Epub 2006 Jun 5. PMID: 17223516.
- Elwany S, Thabet H. Obstruction of the nasal valve. J Laryngol Otol. 1996; 110: 221–224. doi: 10.1017/s0022215100133250.
- Alotaibi A. (2017) The Common Complications after Septoplasty and Septorhinoplasty: A Report in a Series of 127 Cases. International Journal of Otolaryngology and Head & Neck Surgery, 6, 71-78. doi: 4236/ijohns.2017.66010.
- Arslan E, Majka C, Beden V. Combined use of triple cartilage grafts in secondary rhinoplasty. J Plast Reconstr Aesthet Surg. 2007;60 (2):171-9. doi: 10.1016/j.bjps.2006.04.014. Epub 2006 Jul 10. PMID: 17223515.
- Yoo S, Most SP. Nasal airway preservation using the autospreader technique: analysis of outcomes using a disease-specific quality-of-life instrument. Arch Facial Plast Surg. 2011 Jul-Aug;13(4):231-3. doi: 10.1001/archfacial.2011.7. Epub 2011 Feb 21. PMID: 21339471.
- Saedi B, Amali A, Gharavis V, Yekta BG, Most SP. Spreader flaps do not change early functional outcomes in reduction rhinoplasty: a randomized control trial. Am J Rhinol Allergy. 2014 Jan-Feb;28(1):70-4. doi: 10.2500/ajra.2014.28.3991.
- Hassanpour SE, Heidari A, Moosavizadeh SM, Tarahomi MR, Goljanian A, Tavakoli S. Comparison of Aesthetic and Functional Outcomes of Spreader Graft and Autospreader Flap in Rhinoplasty. World J Plast Surg. 2016 May;5 (2):133-8. PMID: 27579268; PMCID: PMC5003948.
- Manavbasi YI, Basaran I. The role of upper lateral cartilage in dorsal reconstruction after hump excision: section 1. Spreader flap modification with asymmetric mattress suture and extension of the spreading effect by cartilage graft. Aesthetic Plast Surg. 2011 Aug; 35 (4):487-93. doi: 10.1007/s00266-010-9641-4. Epub 2011 Feb 7. PMID: 21298515.
- Keyhan SO, Fallahi HR, Cheshmi B, Jafari Modrek M, Ramezanzade S, Sadeghi E. Spreader Graft vs Spreader Flap in Rhinoplasty: A Systematic Review and Meta-Analysis of Aesthetic and Functional Outcomes. Aesthet Surg J. 2022 May 18; 42 (6):590-602. doi: 10.1093/asj/sjab409. PMID: 34864854.
- Naguib, Maged & M, Rifaat & Madian, Yasser & T, Elnahriry & Eldeeb, Wael. (2020). A Comparative Study of Open Septorhinoplasty with Spreader Graft and Auto-Spreader Flap in Patients with Nasal Obstruction. Acta Scientific Otolaryngology. 2. 20-28. 10.31080/ASOL.2020.02.0075.
- Garefis K, Konstantinidis I, Tsetsos N, Garefi M, Nikolaidis V, Markou K. Role of spreader flaps in primary rhinoplasty, functional and aesthetic outcomes: a systematic review. Rhinology. 2022 Apr 1;60 (2):92-101. doi: 10.4193/Rhin21.235. PMID: 35199801.